
112 Maple Avenue
New City, NY 10956
Tel: 845-634-2900

Common Eye Diseases and Conditions
Age-Related Macular Degeneration
Age-related macular degeneration (AMD) is one of the most common causes of poor vision after age 60. AMD is age-related damage of the inacula. The macula is a small area at the center of the retina in the back of the eye that allows us to see fine details clearly and perform activities such as reading and driving. The visual symptoms of AMD involve loss of central vision. While peripheral (side) vision is unaffected, with AMD, one loses the sharp, straight-ahead vision necessary for driving, reading, recognizing faces, and looking at detail.
Although the specific cause is unknown, AMD seems to be part of aging. While age is the most significant risk factor for developing AMD, heredity, blue eyes, high blood pressure, cardiovascular disease, and smoking have also been identified as risk factors. AMD accounts for 90% of new cases of legal blindness in the United States.
Nine out of 10 people who have AMD have atrophic or" dry" AMD. Dry AMD takes many years to develop. Exudative or" wet" AMD is less common, (occurring in one out of 10 people with AND), but is more serious. In the wet form of AMD, abnormal blood vessels may grow in a layer beneath the retina, leaking fluid and blood, and creating distortion or a large blind spot in the center of your vision. If the blood vessels are not growing directly beneath the macula, laser surgery is usually the treatment of choice. The procedure usually does not improve vision but tries to prevent further loss of vision. For those patients with wet AMD whose blood vessels are growing directly under the center of the macula, a procedure called photodynainic therapy (PDT), which causes fewer visual side effects, is sometimes used. Intravitreal injections of certain medications that act against new blood vessels can also be used in these cases.
Certain vitamins were shown to have beneficial effects on the progression of dry AMD) in a study called the Age Related Eye Disease Study, or AREDS. This study showed that daily nutrient supplement of the following regimen helped slow the progression of macular degeneration:
-
Vitamin A(also known as beta carotene) 15 mg
-
Vitamin C 500mg
-
Vitamin E 400 IU
-
Zinc 80 mg
-
Copper 2mg
This regimen is available commercially as Ocuvite or I-Caps. There are many different vitamin formulations with these names, so be sure to check the ingredients and look for the letters AREDS on the label. Family members of patients with macular degeneration may also want to take these vitamins to reduce their risk of developing AMD, as they seem to have a protective effect on the macula.
Blepharitis Lid Margin Disease
Lid margin disease is a common and frequently chronic inflammation of eyelids. Symptoms include irritation, itching, burning, tearing, and, occasionally, a red eye. This condition frequently occurs in people who tend to have oily skin, dandruff, or dry eyes.
Bacteria normally reside on the skin, but in some people, they thrive in the skin at the base of the eyelashes. Nearby oil glands may be Overactive, causing dandruff-like scales AND particles to form along the lashes; and eyelid margins, which can cause redness, stinging, or burning. The symptoms of blepharitis and lid margin disease may fluctuate.
Lid margin disease cannot be cured, but it can be controlled with a few simple, daily hygienic measures, such as the following:
-
At least twice a day, place a warm, wet washcloth over your closed eyelids for a minute. Re wet it as it cools, two or three times. This will soften and loosen scales and debris. More important, it helps liquefy the oily secretions from the eyelids' oil glands, which helps prevent the development of a chalazion, an inflamed lump in an eyelid oil gland.
-
Use a thin, wet washcloth, cotton swab, or commercial lint-free pad soaked with a mild eyelid cleanser (e.g. Ocusoft) or diluted baby shampoo to gently scrub the base of the lashes for about 15 seconds per lid.
When medications are necessary, they may include:
-
A topical antibiotic ointment, usually erythromycin, applied to the lashes and lids at bedtime to decrease bacteria
-
Oral antibiotics, usually doxycycline, to control bacteria
-
Artificial tears (over-the-counter lubricant eyedrops) to relieve symptoms of dry eye
-
A short course of steroid eyedrops to decrease inflammation
Medications alone are not sufficient to control lid margin disease. The application of warm compresses and daily cleansing of the eyelids and lashes are essential to controlling symptoms.
Floaters and Flashes
Small specks or clouds moving in your field of vision as you look at a blank wall or a clear blue sky are known as floaters. Most people have some floaters normally but do not notice them until they become numerous or more prominent.
In most cases, floaters are part of the natural aging process. Floaters look like cobwebs, squiggly lines, or floating bugs. They appear to be in front of the eye but are actually floating inside. As we get older, the vitreous (the clear, gel-like substance that fills the inside of the eye) tends to shrink slightly and detach from the retina, forming chimps within the eye. What you see are the shadows these clumps cast on the retina, the light-sensitive nerve layer lining the hack of the eye.
The appearance of flashing lights comes from the traction of the vitreous gel on the retina at the time of vitreous separation. Flashes look like twinkles or lightning streaks.Floaters can get in the way of clear vision, often when reading. Try looking up and then down to move the floaters out of the way. While some floaters may remain, many of them will fade over time.
Floaters and flashes are sometimes associated with retinal tears. When the vitreous shrinks, it can pull on the retina and cause a tear or hole. A retinal tear or hole usually requires treatment with a laser to prevent it from leading to a more serious condition, such as a retinal detachment. If new floaters appear suddenly, if you you see sudden flashes of light, or if you notice a shadow in the eye, see an ophthalmologist immediately.
Pterygium and Pinguecula
A pterygium is a mass of fleshy tissue that grows over the cornea (the clear front window of the eye). It may remain small or may grow large enough to interfere with vision. A pterygium most commonly occurs on the inner corner of the eye, but it can appear on the outer corner as well.
The exact cause of pterygiais not well understood. They occur more often in people who spend a lot of time outdoors, especially in sunny climates. Long-term exposure to sunlight, especially to ultraviolet (UV) rays, and chronic eye irritation from dry, dusty conditions seem to play an important role. Thy eye also may contribute to pterygium formation.
When a pterygiurn becomes red and irritated, eyedrops or ointments can be used to help reduce the inflammation. If the pterygium grows rapidly or is large enough to threaten sight, it can be removed surgically. Despite proper surgical removal, a pterygium may return, particularly in young people. Protecting the eyes from excessive ultraviolet light with proper sunglasses, avoiding dry, dusty conditions, and using artificial tears can also help.
A pinguecula is a yellowish patch or bump on the white of the eye, most often on the side closest to the nose. It is not a tumor but is an alteration of normal tissue resulting in a deposit of protein and fat. Unlike a pteiygiuni, a pinguecula does not actually grow onto the cornea. A pinguecula can also be a response to chronic eye irritation or sunlight.
No treatment is necessary unless the pinguecula becomes inflamed. A pingueeula does not grow onto the cornea or threaten sight. On rare occasions, a pinguecula can be surgically removed if it is particularly annoying.
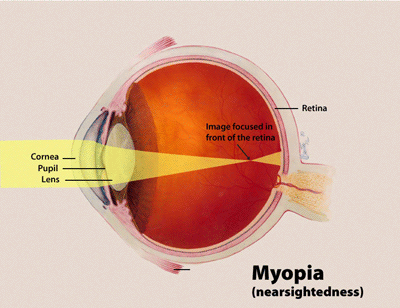
Myopia (Nearsightedness)
Nearsighted individuals typically have problems seeing well at a distance and are forced to wear glasses or contact lenses. The nearsighted eye is usually longer than a normal eye, and its cornea may also be steeper. Therefore, when light passes through the cornea and lens, it is focused in front of the retina. This will make distant images appear blurred. There are several refractive surgery solutions available to correct nearly all levels of nearsightedness.

Hyperopia (Farsightedness)
Farsighted individuals typically develop problems reading up close before the age of 40. The farsighted eye is usually slightly shorter than a normal eye and may have a flatter cornea. Thus, the light of distant objects focuses behind the retina unless the natural lens can compensate fully. Near objects require even greater focusing power to be seen clearly and therefore, blur more easily. LASIK, Refractive Lens Exchange and Contact lenses are a few of the options available to correct farsightedness.
Astigmatism
Asymmetric steepening of the cornea or natural lens causes light to be focused unevenly, which is the main optical problem in astigmatism. To individuals with uncorrected astigmatism, images may look blurry or shadowed. Astigmatism can accompany any form of refractive error and is very common. Astigmatism can be corrected with glasses, contact lenses, corneal relaxing incisions, laser vision correction, and special implant lenses.


Presbyopia
Presbyopia is a condition that typically becomes noticeable for most people around age 45. In children and young adults, the lens inside the eye can easily focus on distant and near objects. With age, the lens loses its ability to focus adequately.
Although presbyopia is not completely understood, it is thought that the lens and its supporting structures lose the ability to make the lens longer during close vision effort. To compensate, affected individuals usually find that holding reading material further away makes the image clearer. Ultimately, aids such as reading glasses are typically needed by the mid-forties. Besides glasses, presbyopia can be dealt with in a number of ways. Options include: monovision and multifocal contact lenses, monovision laser vision correction, and new presbyopia correcting implant lenses.